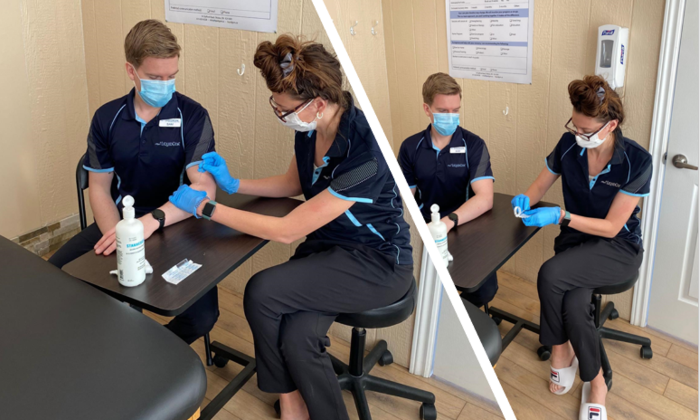
What is Functional Dry Needling?
Functional dry needing (FDN) is a skilled technique performed by a qualified therapist using a filiform (or dry) needle to penetrate into muscles and other tissue to influence the body’s function and help in the treatment of neuromuscular conditions, pain, and dysfunction.
This technique was first proposed for use to stimulate muscles in the early 1930s and started to be widely used in the 1980’s after more research on the topic was published.
Why is it called dry needling?
Because the filiform needles used do not inject a substance into the body, hence “dry needle.” They look more like a pin than a needle, and instead of slicing open the muscle for injection— the way needles do for vaccines and shots—these needles slide in more smoothly.

How does it work?
This is a treatment which uses very thin needles that are inserted into the muscles to help relieve pain, decrease weakness, and increase the range of movement available to a person.
It sounds scary, I know but it really isn’t! Here is why:
-
- The needles are very thin (so thin they could fit on the end of a standard flu shot needle).
- Injection needles are designed to cut into the muscle and open it up so that the injected substance has somewhere to go. Dry needles are designed to slide through the muscle. It is only meant to cause the smallest trauma possible so that it can restart the muscles healing response without causing real lasting damage that needs repair.
- They are done with your friendly chatty physio you see all the time, not some scary nurse or doctor in a lab coat (I am only kidding about the doctors and nurses, they are normally all friendly as well)
Is there a difference between FDN and acupuncture? YES


How does it help?
FDN can help decrease pain, increase range of movement, and increase strength.
FDN acts as a reset for a dysfunctional muscle and its nervous system circuit.
If a muscle is too tight or knotted this will reset it to a more loosened or relaxed state.
If a muscle is under active this can stimulate it to start working again.
How long does it last?
Typically 2-3 days. But if you use this technique along with doing your exercises daily it can last longer and eventually help reverse any disfunction.
Think of it this way:
If you have an appliance (muscle/nerve unit) that is dodgy it will keep throwing the breaker. You can reset the breaker (use FDN to regain neuromuscular balance) but if the faulty appliance still isn’t working it will continue to throw the breaker periodically (pain comes back after a couple days). BUT if you fix the appliance (retrain the muscle) then eventually it will stop throwing the breaker.
What are the benefits?

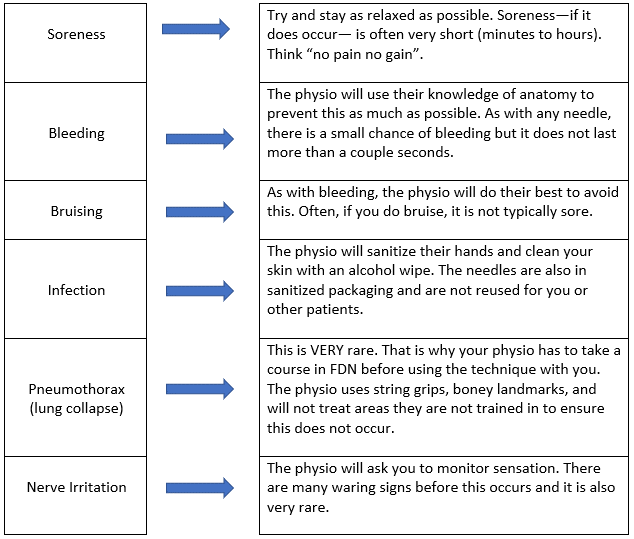
What can go wrong and how do we avoid that?
Is FDN for me?
It might be. It is not a technique that is safe for everyone. For instance, it is not used in the first trimester in pregnancy or for people with bleeding or clotting disorders among other health conditions. Furthermore, if you really dislike needles or have a severe phobia of them it may not be the treatment for you.
Talk to your physiotherapist and discuss whether it is appropriate or not with you.
CALL LIQUIDGYM TODAY TO BOOK WITH ONE OF OUR PHYSIOTHERAPISTS WHO OFFERS FUNCTIONAL DRY NEEDLING AS A TREATMENT OPTION!
613-820-8228
References:
Ahn AC, Colbert AP, Anderson BJ, et al. Electrical Properties of Acupuncture Points and Meridians: A Systematic Review. Bioelectromagnetics. 2008;29:245-256
Boyles, R., Fowler, R., Ramsey, D. and Burrows, E., 2015. Effectiveness of trigger point dry needling for multiple body regions: a systematic review. Journal of Manual & Manipulative Therapy, 23(5), pp.276-293.
Evidence in Motion, Functional Dry needling Level 1 course, 2021.
FSBPT. Analysis of Competencies for Dry Needling by Physical Therapists. Dry Needling Practice Analysis
Gafarov GA. Acupuncture Research Methods. Journal of Applied Biotechnology and Bioengineering. 2020;7(6):276-278
Legge, David. (2014). A History of Dry Needling. Journal of Musculoskeletal Pain. 22. 10.3109/10582452.2014.883041.
Vickers AJ, Cronin AM, Maschina AC, et al. Acupuncture for Chronic Pain: Individual Patient Data Meta-Analysis. Archives of Internal Medicine. 2012;172(19):1444-1453
Author:
Jessica Buffam
Physiotherapist